Key Takeaways
- When evaluating a Cardiology EHR system, consider factors beyond just the initial cost.
- The true expense of a low-cost EHR often manifests as inefficiencies, staff burnout, compliance challenges, and decreased patient satisfaction.
- A comprehensive, scalable EHR may require a larger upfront investment, but it ultimately enhances workflows, elevates patient care, and helps avoid a cycle of additional costs and hidden fees.
- Explore 5 strategies for a seamless Cardiology EHR transition.
Let’s delve into the actual costs associated with starting with a system that merely appears to save you money.
Table of Contents
The True Cost of Implementation
Implementation often reveals the first unexpected costs. With many low-cost EHRs, onboarding is typically minimal, offering little guidance beyond the basics. This results in:
- Insufficient training that leaves staff uncertain about how to use the system effectively
- Increased hours spent troubleshooting rather than focusing on patient care
- Additional fees for “premium” training sessions or extended support
For Cardiology practices, this can be particularly disruptive. Picture your staff struggling to document follow-ups for cardiac procedures or manage patient histories without the appropriate templates. Instead of concentrating on patient care, they find themselves investing extra hours attempting to adapt a generic system to their needs.
Research indicates that with inadequate training, only a fraction of end-users report satisfaction with their EHR. Without proper engagement, achieving successful implementation becomes nearly impossible, and what initially seemed affordable can quickly drain both efficiency and staff morale.
Workflow Disruption: The Hidden Costs
- Documentation delays: Cardiology providers often require specialized templates for echocardiograms, stress tests, or medication management. Generic systems compel providers to engage in time-consuming manual processes.
- Inefficient billing processes: Gaps in revenue cycle management, such as missed codes for cardiac procedures, can lead to claim denials.
- Staff burnout: Excessive clicks, repetitive data entry, and disrupted workflows consume valuable clinical time and contribute to turnover.
Every minute wasted navigating a poorly designed system is a minute not spent with patients. Those “lost minutes” translate directly into lost revenue and a decline in the quality of care provided.
The Hidden Costs: Add-Ons and Fees
- Advanced reporting or analytics (e.g., to monitor patient outcomes)
- Customization of templates and forms for Cardiology-specific procedures
- Secure messaging or patient portal access
- E-prescribing capabilities, particularly for controlled substances
What initially appeared to be an affordable EHR for Cardiology practices can quickly escalate into a system that costs more than premium alternatives—without delivering comparable value.
Cardiology-Cloud’s comprehensive EHR system addresses these challenges by providing reporting, e-prescribing, customization, and patient portal access from the outset.
Telehealth and Fragmented Services
In today’s healthcare landscape, telehealth is essential for ensuring patient access. However, with a low-cost EHR, you may find that telehealth tools are offered as expensive add-ons or, worse, are completely unavailable.
For Cardiology clinics, managing multiple systems for patient follow-ups, post-operative consultations, and routine care can be a daunting task. This not only leads to increased subscription expenses but also heightens compliance risks and hampers overall efficiency.
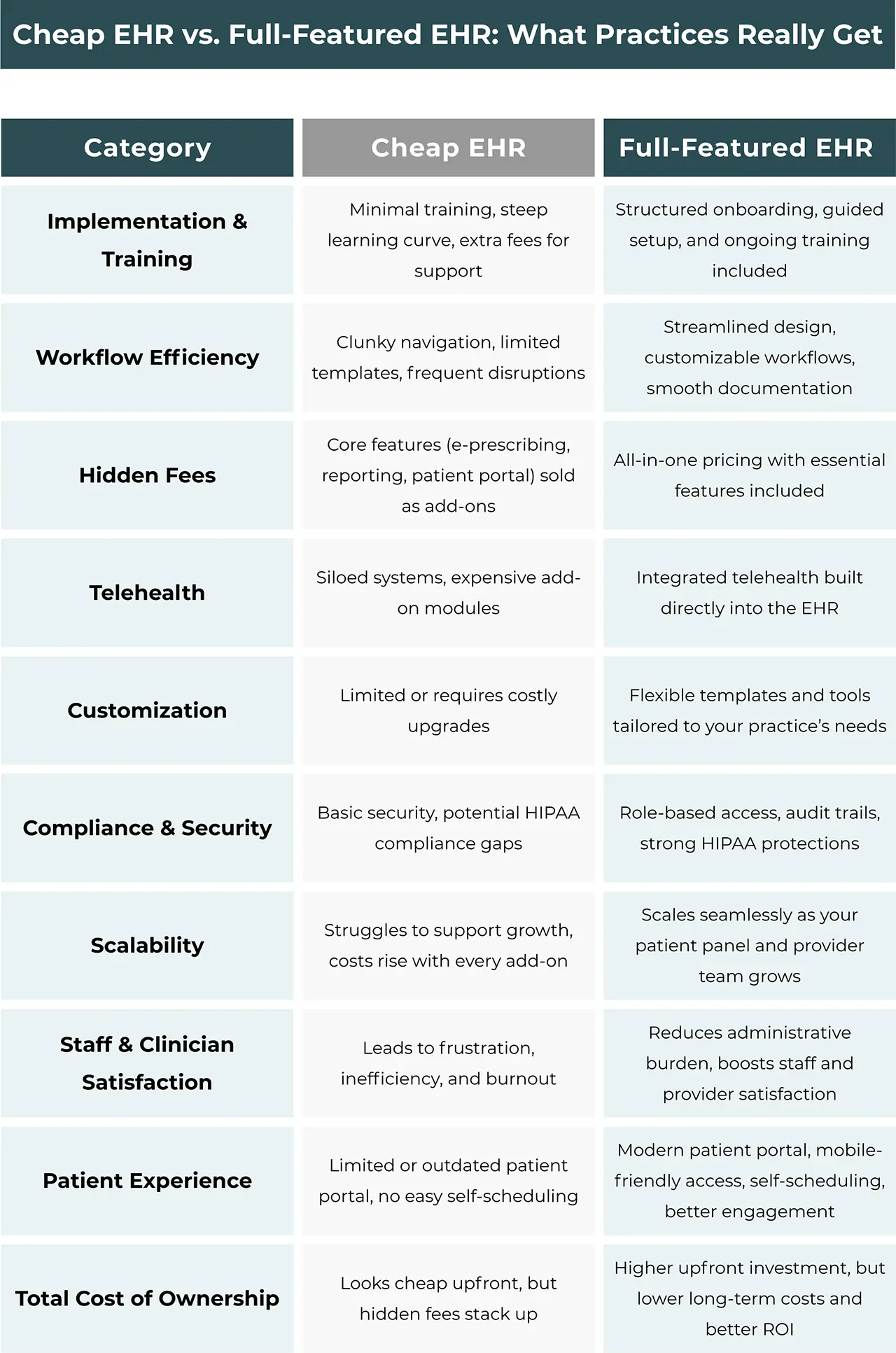
How Much Does a Cardiology EHR Cost, Really?
Determining the cost of a Cardiology EHR involves more than just the initial price tag; it requires a comprehensive understanding of the total cost of ownership (TCO):
- Direct costs: Licensing, setup, support, and training
- Indirect costs: Decreased staff productivity, patient no-shows, billing inaccuracies, and turnover due to burnout
- Growth costs: Additional fees for every new provider, feature, or integration as your practice expands
What a Full-Feature EHR Provides From Day One
A comprehensive Cardiology EHR is designed to support your practice from the outset, ensuring you have the tools necessary for success. This includes:
- Free implementation support – Tailored Cardiology workflows, templates, and settings are configured correctly from day one, ensuring a smooth transition.
- Comprehensive training – Proper training can lead to an impressive 83% of end-users reporting satisfaction, compared to only 36% without it.
- Data migration included – Seamless transfer of patient records, demographics, and historical notes without incurring extra costs.
- Practice-specific customization – Cardiology-focused templates for various care types streamline processes and enhance efficiency.
- Ongoing support at no extra charge – Responsive customer service and continuous training keep your staff well-informed and capable.
The distinction is evident: rather than being charged for basic services, you gain a partner dedicated to your long-term success.
Choosing Wisely: Invest in Long-Term Value
Instead of inquiring about “free EHR options,” consider asking:
- Will this system scale as my Cardiology practice grows?
- Does it include specialty-specific tools for Cardiology care?
- Are telehealth, patient engagement, and reporting features integrated or sold separately?
- What level of support and training is included?
Investing in a robust EHR tailored specifically for Cardiology practices is more about value than mere cost. The right solution not only supports your growth but also enhances clinician satisfaction and ensures that patients receive the quality care they deserve.











